A recent VA pilot study shows promise for early detection and treatment of an eye disease that affects many with diabetes. About a quarter of VA patients have diabetes.
Anyone who has the disease can develop diabetic retinopathy. It involves damage to the light-sensitive tissue in the back of the eye—the retina.
Diabetic retinopathy is a leading cause of blindness among working-age Americans. “This means vision loss is disrupted when these people are at the peak of their wage-earning potential,” says Dr. Machelle Pardue. She is associate director of the Center for Visual and Neurocognitive Rehabilitation at the Atlanta VA Medical Center.
Pardue recently led a pilot study of a hand-held electroretinogram (ERG) device to detect pre-clinical, or early stage, diabetic retinopathy. The study also looked at the drug Levodopa—usually used for Parkinson’s disease—to treat patients with early signs of the condition.
Device detects early retinal problems
Pardue and her team found that the device, the RETeval, has the sensitivity to detect early retinal problems in diabetic patients prior to “clinically recognized vascular changes.”
“Let’s say we’re able to detect diabetic changes in the eye within the first five years. That’s still around 10 years before it’s clinically diagnosed.”
“These data demonstrate the potential to use this approach as a new screening method for diabetic retinopathy that would detect retinal defects much earlier than the currently used fundus photography,” the researchers write. That procedure calls for photographing the rear of the eye and recording activity in the retina.
The researchers also determined that Levodopa can restore retinal function to normal within two weeks and can continue to provide benefit for at least two weeks after treatment.
The results appeared online in February 2020 in the journal Diabetes, published by the American Diabetes Association.
Catching changes within the first five years
“Let’s say we’re able to detect diabetic changes in the eye within the first five years,” says Pardue. “That’s still around 10 years before it’s clinically diagnosed. That’s a big difference. When you’re at that late stage of the disease, a lot of drugs, no matter how good they are, just aren’t going to be able to treat it effectively because the disease has progressed too far. So there are sweet spots where diseases are reversible and treatable.”
To read more about the study, visit VA Research Currents.
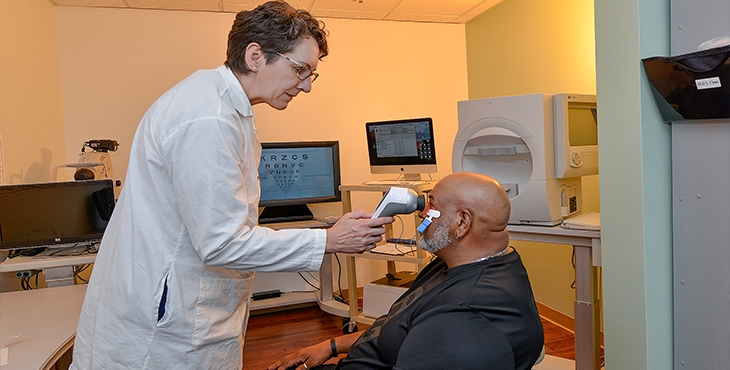
Photo at top: Dr. Machelle Pardue performs an electroretinogram on Army Veteran Michael Brooks, who participated in her study. (Photo by Joey Rodgers)
Topics in this story
More Stories
Diverse representation of women in health care research allows MVP to make discoveries for women’s health
Join the Million Veteran Program online. You will have the option to receive an at-home blood sample collection kit in the mail.
VHA's new podcast series, New Horizons in Health, features a candid discussion of psychedelic assisted therapies for Veterans experiencing mental health conditions.






Thank you
I don’t have Diabetes (or diagnosed yet) but have Parkinson’s Disease and My Left eye has Macular Degeneration which I’m having a lot of vision distortion and a blind spot in the center of the eye and right eye at times indicates with visual test a 20/20 -20/30 but some of the time through using muscular squinting can get a 20/20 but still hard to focus as I have lost my “Depth Perception” do to the Left Eye due to Macular condition. I don’t take anything for my PD but could the Meds for Parkinson’s help this as well?
I’m 78 Years old and body is breaking down as well as falling and have 9 screws in this side, 3 in my RT Hip broken at the neck of the hip joint and 4 in my RT foot arch w/plate and 2 in my heal joint. I have been “Flat-Footed” ALL my life but the fallen arch happened when I was about 38 years old. Trying to give you as much information as possible! I hope it helps! I would like to get back to LIVING again and serving our country volunteering with the knowledge I have gained in my lifetime.
Is there a similarity to my advancing glaucoma?
I am a 20% disabled type 1 diabetic treated at the Atlanta VA Medical Center. In 2008 I was prescribed Travaprost Z 0.0$5 to treat the glaucoma that was building as my eye pressure was increasing. That medication caused my eyes to bleed. Another ophthamologist prsecribed levobunolol, HCL after I called the VA eye clinic to let them know about the bleeding eyes. That doctor obviously didn’t look to see that I was a type 1 diabetic and levobunolol has a beta-blocker in it. After 4 911 calls in two years I learned that the beta blocker hides hypgblycimia which was the reasons for the ambulance calls. As a result, I now see a private opthamologist for my eye care.