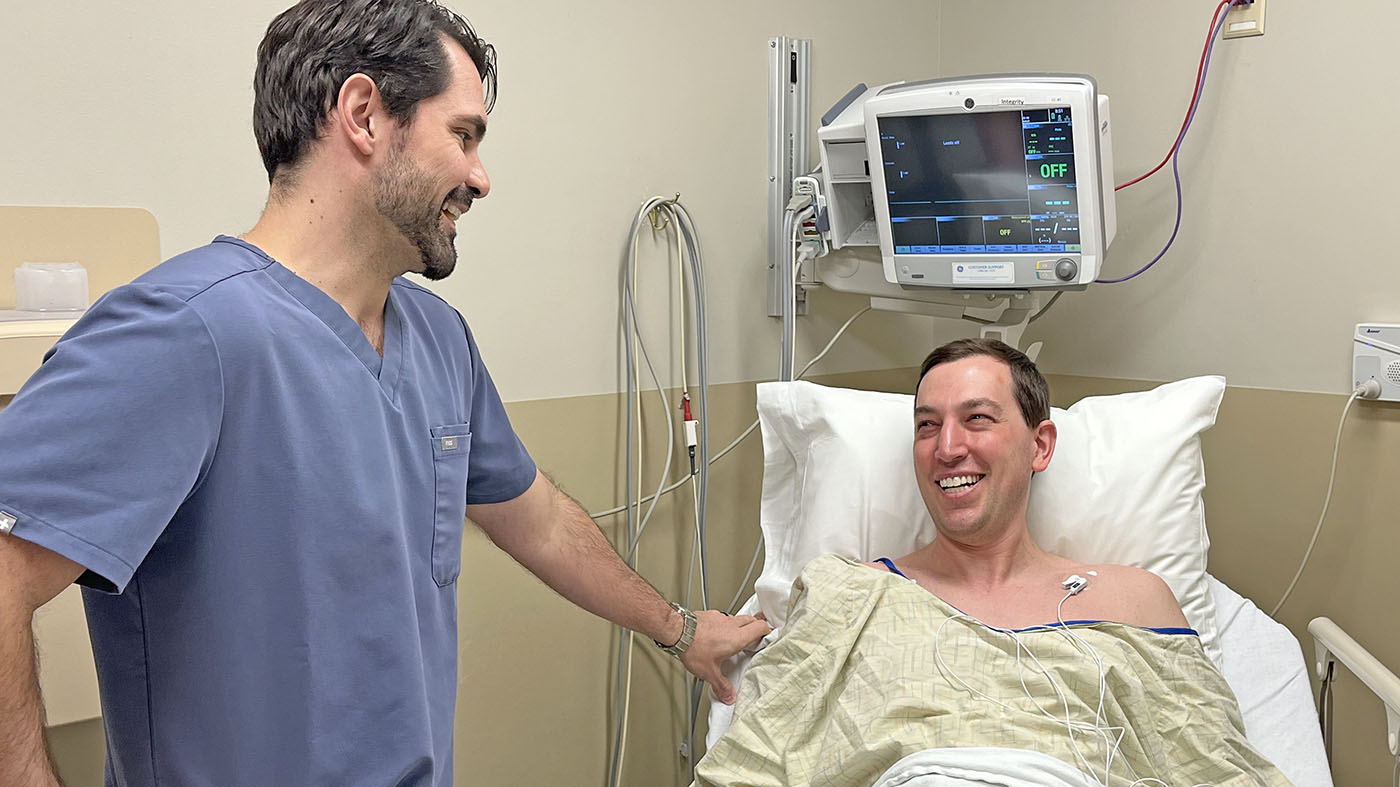
To the VA North Texas Health Care System, COVID-19 is more than just a disease, it’s a challenge that has tested the readiness of the Mental Health Program and forced it to evolve.
“Back in March 2020, it started to become apparent that COVID-19 was going to be here for a while,” said Martin Barrick, a mental health integration social worker. “We had to adapt the way we delivered mental health care. We had to figure out how to care for Veterans who are already under a lot of stress while minimizing the risk of catching and spreading this disease.”
VA began piloting telehealth technology in the 1990s and has grown to become the largest provider of telehealth services in the United States. VA provides telehealth services to any Veteran who qualifies for VA health care and who lives in the U.S or a U.S. territory.
Once seen as technology secondary to in-person visits or to reach Veterans living in rural areas, tele-mental health care is now the primary method of delivering mental health care access to Veterans. In 2020, VA North Texas saw nearly 40,000 unique mental health patients and accounted for nearly 115,000 tele-mental health appointments.
Pictured above, Barrick, conducts a tele-mental health visit with a Veteran through VA Video Connect.
VA ahead of the curve
“Thankfully, our mental health department was ahead of the curve,” said Kristen Backe, a PharmD and mental health clinical pharmacy specialist. “It (VA) had already been doing telehealth appointments. We increased access to mental health care, medication management and counseling for patients who may not have otherwise had it. Patients who live far away, don’t have transportation, have work or school during normal business hours, are now able to see providers virtually instead of having to come in person for every visit.”
The availability of this technology made it easier to adapt to a changing landscape, but it also came with its own challenges.
“Comprehensive mental health care is not just about the words a Veteran says but their facial expressions, body language, and overall presentation,” said Lindsey Cooper, ssychologist and PTSD/SUD Mental Health Trauma Services. “Providing services virtually limited our access to some of these important observations and required us to think outside the box.”
In-person and walk-in services still available
Throughout every stage of the pandemic, VA North Texas still made in-person appointments and walk-in services available for Veterans seeking mental health care.
“We never closed,” said Cooper. “We continued to see Veterans every day and we were even able to supply them with iPads and cell phones so they could attend appointments virtually. Additionally, we utilized the telephone as backup if the video technology failed.”
Among other tools that VA developed to help Veterans cope during the pandemic is the COVID Coach App. The app was created for everyone, including Veterans and service members, to support self-care and overall mental health care during the COVID-19 pandemic. It is available in English and Spanish.
According to Cooper, Veterans need to monitor their mental health as much as their physical health and seek help when needed.
“Today, there are more online resources available to Veterans and their families than ever before and VA truly encourages Veterans to make their mental health a priority.”
Jesus Flores is a public affairs specialist for the VA North Texas Health Care System.
Topics in this story
More Stories
VA promotes early nutrition intervention for chronic kidney disease with targeted programs like Heathier Kidneys Through Your Kitchen.
VA Research Advisory Committee on Gulf War Veterans’ Illnesses hosting Veteran Engagement Sessions in Phoenix for 1990-91 Gulf War Veterans.
Navy Veteran and president of the American Medical Association got a colonoscopy and encourages other Veterans to do the same.