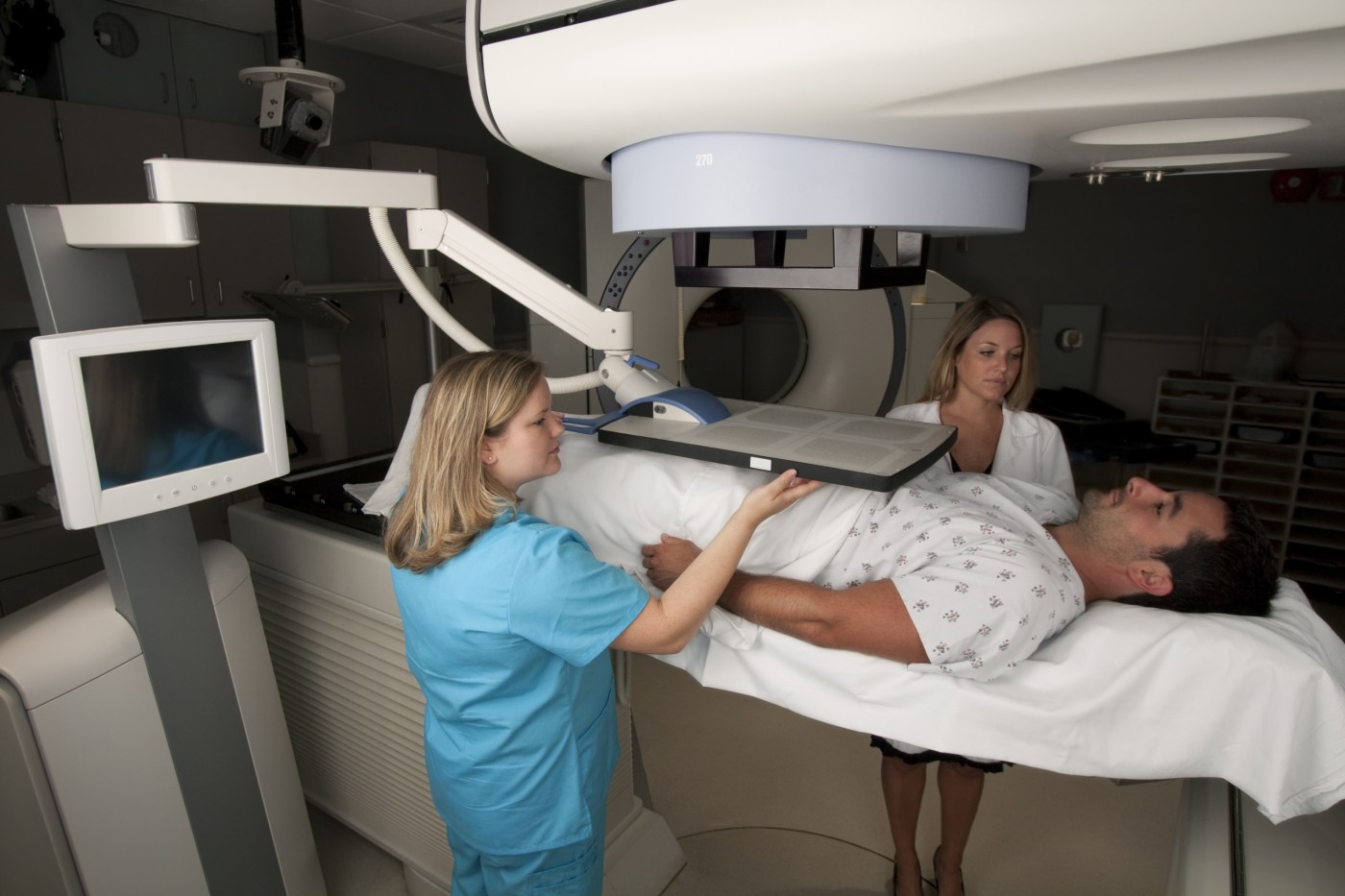
Prostate cancer has historically been considered incurable once it has spread to parts of the body distant from the prostate gland itself. Now, a VA study called STARPORT is examining an innovative treatment approach for men whose prostate cancer has spread to a limited number of distant areas despite initial treatment with surgery or radiation.
“Improved treatments are needed for these men whose prostate cancer has spread and who are left without a lifesaving option,” says Dr. Abhishek Solanki. “Promising evidence suggests that men with limited areas of spread may benefit from adding radiation or surgery that targets metastatic lesions to today’s standard treatment with hormones.”
Solanki is a radiation oncologist and researcher with the Hines VA hospital and Loyola University Medical Center in Chicago. He is the lead investigator of a multisite clinical trial funded with $8.6 million through VA’s Cooperative Studies Program. The trial is known by the acronym VA STARPORT. It stands for STAndard Systemic TheRapy With or Without PET-directed Local Therapy for OligoRecurrenT Prostate Cancer.

Dr. Abhishek Solanki, a radiation oncologist and researcher at the Hines VA in Chicago, is leading the VA STARPORT trial.
Focus on cancer with limited spread
Solanki summarizes the goal of the trial: “VA STARPORT is designed to provide more definitive evidence of whether local therapy along with systemic treatments will lead to better outcomes for some Veterans with limited spread of their prostate cancer.”
Prostate cancer is the most commonly diagnosed cancer among Veterans in VA. It accounts for nearly a third of cancer diagnoses. Prostate cancer is often found early and cured with treatments such as surgery or radiation. But some patients’ cancer spreads and becomes life-threatening.
Cancer that has spread, or metastasized, is typically treated with “standard systemic therapy” (SST) that affects the entire body to slow disease progression. The cornerstone of this approach is hormone therapy to suppress testosterone.
Turning metastases Into targets
VA STARPORT is based on a growing scientific understanding that prostate cancer can spread beyond the prostate itself yet not fan out uncontrollably through the body. By targeting defined areas of metastasis, aggressive local therapy – surgery or radiation – might be capable of diminishing further spread in “oligometastatic,” or “oligorecurrent,” cancer. Such therapy might even help eradicate the cancer altogether in some patients, Solanki says.
The prefix “oligo,” from Greek, means “a few.” The term “oligorecurrent,” as defined in this study, refers to cancer that has spread to no more than five areas.
To pinpoint the metastatic lesions’ locations and target these areas for treatment as precisely as possible, researchers will use sophisticated positron emission tomography (PET) imaging technology approved by the U.S. Food and Drug Administration in recent years.
Identify patients with `previously invisible’ metastatic disease
For example, one PET imaging technology, expected to become widespread within the VA health care system this year, is called “prostate-specific membrane antigen,” or PET. It is significantly more accurate than prior imaging options.
“With this technology, we will be able to identify many patients who have metastatic disease that was previously invisible,” explains Dr. Nicholas Nickols, a radiation oncologist specializing in prostate cancer care and research at the VA Los Angeles Health Care System. He is the local site investigator for VA STARPORT in Los Angeles.
Along with these types of groundbreaking advances in imaging and the increased understanding of oligometastasis has also come improved precision in radiotherapy. Clinicians are now able to safely deliver targeted radiation treatment to virtually anywhere within the body, explains Nickols.
More Information
Click here to read the full story.
Click here to learn more about the study.
Click here to learn more about VA research.
Topics in this story
More Stories
Diverse representation of women in health care research allows MVP to make discoveries for women’s health
Join the Million Veteran Program online. You will have the option to receive an at-home blood sample collection kit in the mail.
VHA's new podcast series, New Horizons in Health, features a candid discussion of psychedelic assisted therapies for Veterans experiencing mental health conditions.